Know Your Worth and Get Paid Right
Know your market value salary with insights across roles, from individual jobs to executive pay and overall company compensation trends. Salary.com lets you to compare costs across cities and stay updated on minimum wage laws to make smarter financial decisions.
Discover your "real" market value using our salary estimator. Find out what your salary should be in just a few clicks.
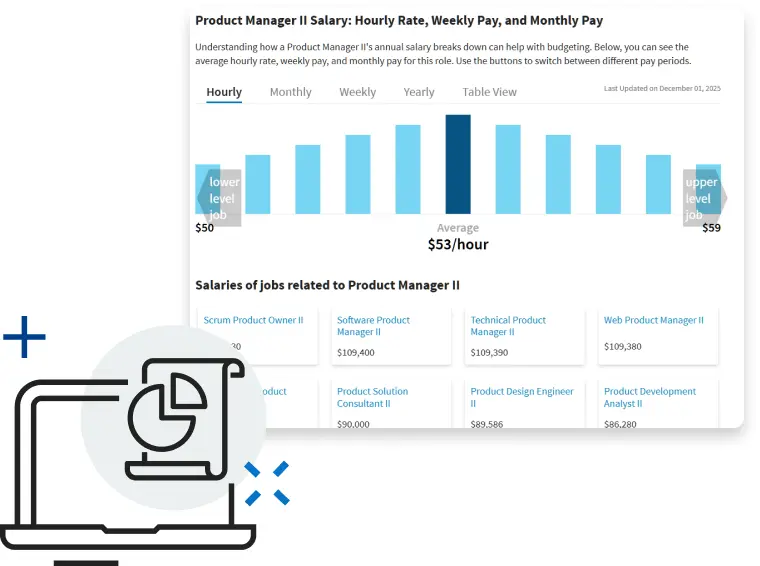
Job Salary
View detailed job salaries and salary estimates across industries and positions. Stay updated on pay trends, earning potential, and key factors that influence salaries to make informed career decisions and reach professional goals.
LEARN MORECompany Salary
See how companies pay across industries, from average salaries for different roles to benefits and compensation trends. Use this salary comparison tool to get the insights needed to make informed career choices and understand how pay is structured.
LEARN MORE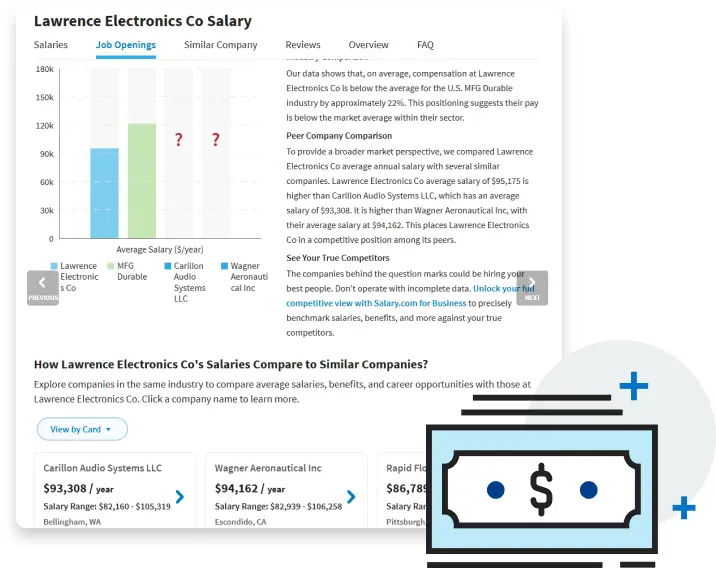
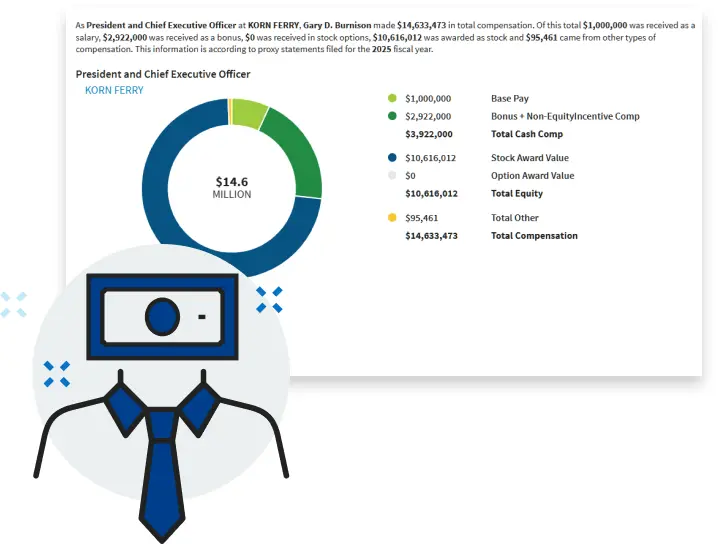
Executive Salary
Get up-to-date executive salary data and see how pay is trending across industries. Whether negotiating an offer or planning your next career move, these pay reports help you make smarter decisions in the executive job market.
LEARN MORECost of Living Calculator
Thinking about relocating? Use our Cost of Living Calculator to compare expenses across cities based on your salary. From housing and utilities to groceries and transportation, see how far your money will go before you relocate.
LEARN MORE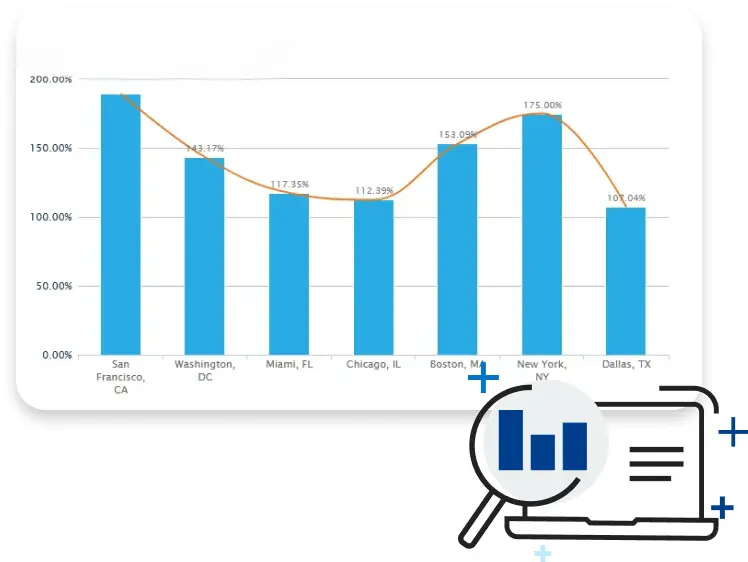
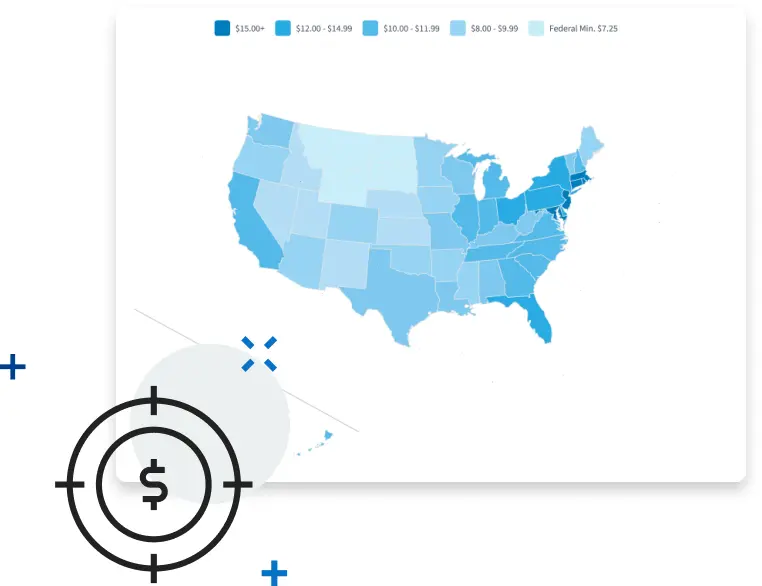
Minimum Wage
Check current minimum wage information across the U.S., including rates for states, cities, counties, and municipalities. This minimum salary checker makes it easy to compare pay by location and stay informed about current labor rules.
LEARN MOREFind Your Ideal Job
Career.com helps you discover job opportunities, connect with roles that fit your skills, and move your career forward. Get personalized recommendations, expert tips, and resources to grow professionally—quick, easy, and free!
Explore JobsFor Employers
Salary.com helps organizations manage market pricing, pay equity, job structures, and compensation planning. Connect with HR systems to ensure pay is fair, competitive, and efficient.
Compensation Datasets
Access trusted and accurate data to confidently price jobs. Salary.com's CompAnalyst Market Data, SalaryIQTM, Compdata and IPAS Surveys keep you competitive and informed across roles and locations.
Compensation Management
CompAnalyst® simplifies your entire compensation process and analyzes your pay practices. Automate survey participation, build and manage salary structures, and quickly identify pay discrepancies and employee flight risks.
Compensation Planning
Ditch manual processes for smarter workflows. CompXL simplifies planning with secure, scalable tools—perfect for even the most complex merit & incentive calculations.
Job Architecture
Simplify job architecture with JobArchitect®. Create, edit, and manage job descriptions in one centralized platform, all while ensuring consistency, compliance, and alignment with roles and skills to stay ahead of workforce needs.
Pay Equity Analytics
Commit to fair pay with the CompAnalyst® Pay Equity Suite. Identify disparities, maintain compliance, and implement strategies for equitable compensation practices.
Pay Communications
Boost trust and retain talent with clear, confident pay communication. Elevate by Salary.com® helps you balance transparency and confidentiality to avoid compensation frustrations.


